The Respiratory System:
Lecture Objectives, Chapter 15: Respiratory SystemUpon completion of this chapter, you should be able to:
Lab Objectives, Exercises 24 and 25, Structure of the Respiratory System and Pulmonary Ventilation: Upon completion of these exercises, you should be able to:
- Discuss the major structures and functions of the respiratory system.
- List the major organs of the respiratory system and describe the functions of each.
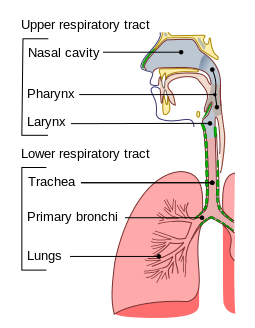
- Differentiate between the structures of the upper and lower respiratory tracts.
- Compare and contrast and explain the mechanism responsible for the exchange of gases that occurs during external and internal respiration.
- List and discuss the volumes of air exchanged during pulmonary ventilation.
- Identify and discuss the mechanisms that regulate respiration.
- Identify several respiratory diseases and conditions that affect the human body.
Lab Objectives, Exercises 24 and 25, Structure of the Respiratory System and Pulmonary Ventilation: Upon completion of these exercises, you should be able to:
- Locate and identify the organs of the respiratory system.
- Describe the structure and function of the respiratory system organs.
- Trace the path of air from the nose to the alveoli.
- Identify the parts of the upper and lower respiratory tracts.
- Explain how changes in the thoracic and lung volumes and lung pressures result in pulmonary ventilation.
- Define and measure or calculate lung volumes and capacities.
- Understand the purpose of a bell jar and how it represents pulmonary ventilation.
- Explain the purpose and basic principles of spirometry and the following medical terms related to this test: tidal volume, inspiratory reserve volume, expiratory reserve volume, residual volume, inspiratory capacity, functional residual capacity, vital capacity, total lung capacity.
- Name the respiratory muscles involved in respiration.
Gross Anatomy of the Respiratory Organs:
The respiratory system moves air into and out of the body. It is the site where oxygen diffuses into the bloodstream, and carbon dioxide diffuses out of the bloodstream to be exhaled.
1. NOSE
Nasal bones - form the base of the nose
Hyaline cartilage - anterior portion
External nares - nostrils x2 are the openings for air to enter a space
Nasal cavity - space lined with mucous membrane
Nasal septum - separates the nasal cavity into right and left portions
Nasal conchae - turbinates, 3 curved structures that are bony and extend into the nasal cavity to warm and moisten and humidify entering air
Meatus - cavities located beneath each nasal concha that increase surface area in the nose
Hard palate - bone that forms the floor of the nasal cavity
Soft palate - soft tissue that connects to the hard palate and from which the uvula hangs down
Internal nares - found at the junction of the hard and soft palates, and are two openings which lead into the posterior nasal pharynx
Paranasal sinuses - frontal, maxillary, ethmoidal and sphenoidal bones have mucous membranes lining these air-filled cavities with ducts that drain into the nasal cavity
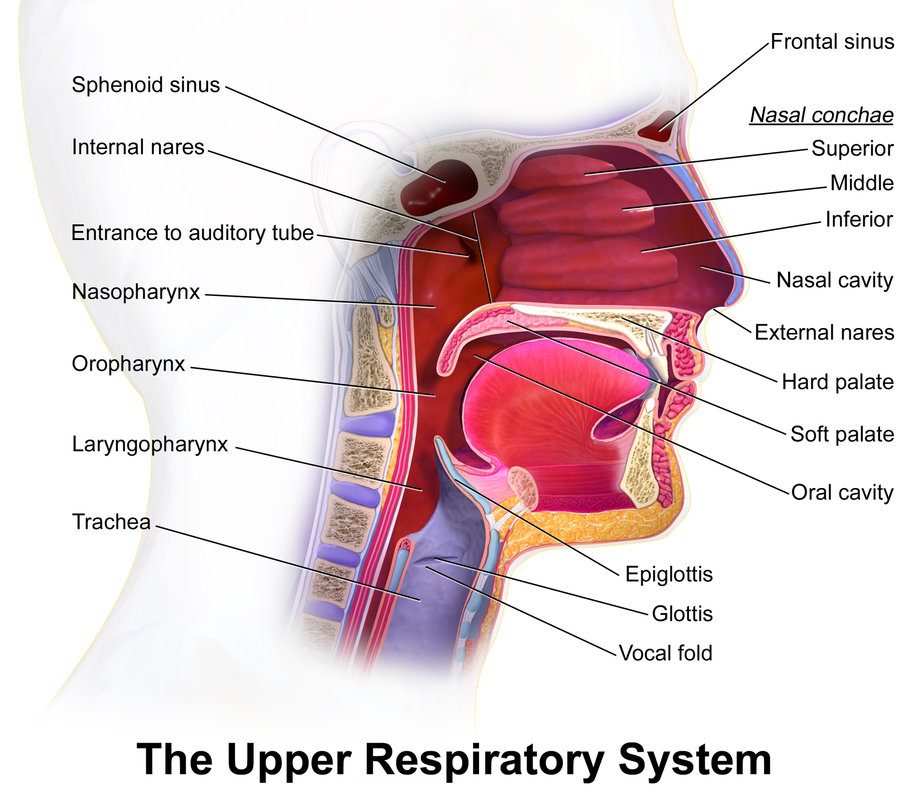
2. PHARYNX
Pharynx - throat; divided into three regions:
1. Nasopharynx - nose; begins at the internal nares and ends at the soft palate
2. Oropharynx - mouth; begins at the soft palate and extends to the level of the hyoid bone
3. Laryngopharynx - larynx; begins at the hyoid bone and extends to the beginning of the esophagus; there is a flap here that closes to prevent food and air from entering the trachea, or windpipe. If air enters, we get the "hiccups". If food or drink enters, we cough or gag or even choke.
Auditory tubes - Eustachian tubes from the ear that connect the middle ear and the nasopharynx. If bacteria travels from the throat to the ear, an ear infection can occur. If it travels from the ear to the throat, Strep Throat can occur.
Pharyngeal tonsil - adenoid; located in the posterior wall of the nasopharynx.
Palatine tonsils - palate tonsils in the back of the throat
Lingual tonsils - tongue tonsils on the sides of the tongue
Soft palate - muscular and found in the oropharynx posterior to the bony hard palate
Uvula - oval-shaped; dangles inferiorly as an extension of the soft palate. During swallowing, this structure pushes superiorly to close off the nasopharynx and to direct food toward the laryngopharynx.
Mucous membranes - line the nose, paranasal sinuses, pharynx, and middle ear are connected by ducts. Infections can spread easily to adjacent areas.
3. LARYNX
Larynx - voice box; connects the laryngopharynx with the trachea
Thyroid cartilage - largest cartilage of the larynx; shield-shaped; seen anteriorly and has a prominence called the "Adam's apple" that is made of hyaline cartilage.
Cricoid cartilage - ring-like; inferior to the thyroid cartilage; larger on the posterior side than on the anterior side; consists of hyaline cartilage; This is the only cartilage that is a complete ring in the larynx or trachea.
Epiglottis - oval-shaped structure that serves as a flap to close over the glottis during swallowing.
Glottis - vocal folds (true vocal cords) and the slit-like opening between them that allows air into the trachea (windpipe).
Complete Activity 1: Nose, Pharynx and Larynx
The respiratory system moves air into and out of the body. It is the site where oxygen diffuses into the bloodstream, and carbon dioxide diffuses out of the bloodstream to be exhaled.
1. NOSE
Nasal bones - form the base of the nose
Hyaline cartilage - anterior portion
External nares - nostrils x2 are the openings for air to enter a space
Nasal cavity - space lined with mucous membrane
Nasal septum - separates the nasal cavity into right and left portions
Nasal conchae - turbinates, 3 curved structures that are bony and extend into the nasal cavity to warm and moisten and humidify entering air
Meatus - cavities located beneath each nasal concha that increase surface area in the nose
Hard palate - bone that forms the floor of the nasal cavity
Soft palate - soft tissue that connects to the hard palate and from which the uvula hangs down
Internal nares - found at the junction of the hard and soft palates, and are two openings which lead into the posterior nasal pharynx
Paranasal sinuses - frontal, maxillary, ethmoidal and sphenoidal bones have mucous membranes lining these air-filled cavities with ducts that drain into the nasal cavity
2. PHARYNX
Pharynx - throat; divided into three regions:
1. Nasopharynx - nose; begins at the internal nares and ends at the soft palate
2. Oropharynx - mouth; begins at the soft palate and extends to the level of the hyoid bone
3. Laryngopharynx - larynx; begins at the hyoid bone and extends to the beginning of the esophagus; there is a flap here that closes to prevent food and air from entering the trachea, or windpipe. If air enters, we get the "hiccups". If food or drink enters, we cough or gag or even choke.
Auditory tubes - Eustachian tubes from the ear that connect the middle ear and the nasopharynx. If bacteria travels from the throat to the ear, an ear infection can occur. If it travels from the ear to the throat, Strep Throat can occur.
Pharyngeal tonsil - adenoid; located in the posterior wall of the nasopharynx.
Palatine tonsils - palate tonsils in the back of the throat
Lingual tonsils - tongue tonsils on the sides of the tongue
Soft palate - muscular and found in the oropharynx posterior to the bony hard palate
Uvula - oval-shaped; dangles inferiorly as an extension of the soft palate. During swallowing, this structure pushes superiorly to close off the nasopharynx and to direct food toward the laryngopharynx.
Mucous membranes - line the nose, paranasal sinuses, pharynx, and middle ear are connected by ducts. Infections can spread easily to adjacent areas.
3. LARYNX
Larynx - voice box; connects the laryngopharynx with the trachea
- Consists of 9 hyaline cartilage rings
- Houses the vocal cords
- Contains 3 small paired cartilages located in the posterior wall of the larynx
- Contains 3 single cartilages (thyroid, cricoid, and epiglottis), comprising the main body of the larynx
Thyroid cartilage - largest cartilage of the larynx; shield-shaped; seen anteriorly and has a prominence called the "Adam's apple" that is made of hyaline cartilage.
Cricoid cartilage - ring-like; inferior to the thyroid cartilage; larger on the posterior side than on the anterior side; consists of hyaline cartilage; This is the only cartilage that is a complete ring in the larynx or trachea.
Epiglottis - oval-shaped structure that serves as a flap to close over the glottis during swallowing.
Glottis - vocal folds (true vocal cords) and the slit-like opening between them that allows air into the trachea (windpipe).
Complete Activity 1: Nose, Pharynx and Larynx
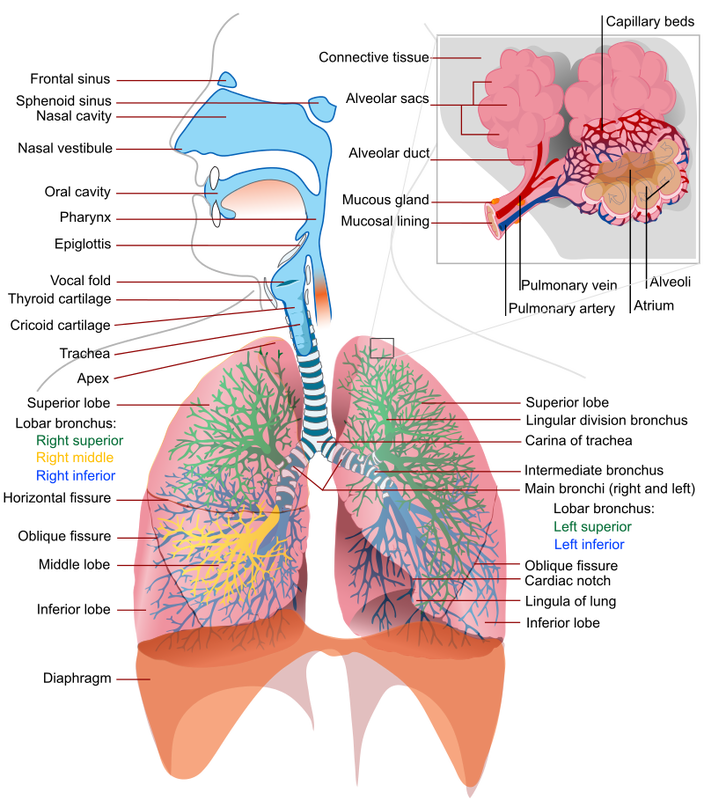
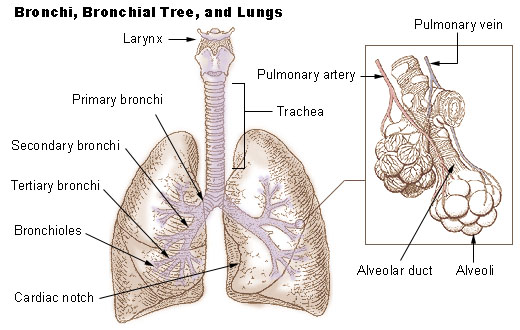
4. BRONCHIAL TREE:
Bronchial tree - lower airways, just like a tree trunk with branches, twigs and fruit, have a trachea, bronchi, bronchioles, and alveoli.
Trachea - windpipe; tube-like conduit that conducts air from the larynx to the bronchi, which is located anterior to the esophagus. It can be palpated with your hand on the surface of your neck.
Tracheal cartilages - C-shaped cartilages that keep the airway open.
Right and left primary bronchi - trachea branches into these structures, of which the right is shorter and the left is longer, each serving the corresponding lung.
Secondary bronchi - lobar; supply a lobe of each lung. There are 3 secondary bronchi on the right, and two secondary bronchi on the left.
Tertiary bronchi - segmental; branch off the secondary bronchi; divide into bronchioles, each serving small compartments of the lung called lobules.
Terminal bronchioles - end brochioles that branch into respiratory bronchioles that begin the respiratory zone of the lung, and branch into alveolar ducts.
Alveolar ducts - lead from the respiratory bronchioles into clusters of alveoli called alveolar sacs.
Alveoli - air sacs of the lungs that bud off like individual grapes of a grape cluster, to increase the surface area for exchange of O2/CO2. If damaged or if they burst/bust open, this results in COPD or emphysema, which can be caused by smoking, asbestos exposure, second-hand smoke exposure, smoke inhalation, long-term mold exposure to a toxic mold, microplastics exposure, and others.
Asthma - a tightening and increase in mucous production of the bronchi
Bronchitis - inflammation of the bronchi
Bronchiolitis - inflammation of the bronchioles
5. LUNGS
Lungs - two lungs are divided into 3 lobes on the right side, and 2 lobes on the left side:
Apex - rounded superior part of the long
Base - broader inferior part of the lung that rests on the diaphragm
Hilus - area of the lung surrounded by pleura, where the bronchi, lymphatic vessels, and nerves enter or exit the medial side of the lung
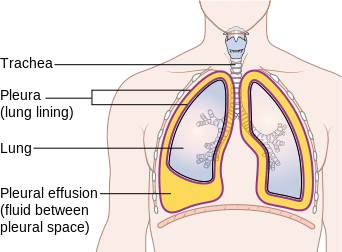
Parietal pleura - lines the thoracic cavity wall
Visceral pleura - covers each side of the lung surface
Pleural cavity - space between the two pleural layers that contains pleural fluid
Pleurisy - inflammation of the pleura
Pneumonia - infection of the lungs (bacterial, viral, fungal or parasite)
Pneumothorax - deflation of the lung
Complete Activity 2: Bronchial Tree and Lungs
Complete Reviewing Your Knowledge Questions
Bronchial tree - lower airways, just like a tree trunk with branches, twigs and fruit, have a trachea, bronchi, bronchioles, and alveoli.
Trachea - windpipe; tube-like conduit that conducts air from the larynx to the bronchi, which is located anterior to the esophagus. It can be palpated with your hand on the surface of your neck.
Tracheal cartilages - C-shaped cartilages that keep the airway open.
Right and left primary bronchi - trachea branches into these structures, of which the right is shorter and the left is longer, each serving the corresponding lung.
Secondary bronchi - lobar; supply a lobe of each lung. There are 3 secondary bronchi on the right, and two secondary bronchi on the left.
Tertiary bronchi - segmental; branch off the secondary bronchi; divide into bronchioles, each serving small compartments of the lung called lobules.
Terminal bronchioles - end brochioles that branch into respiratory bronchioles that begin the respiratory zone of the lung, and branch into alveolar ducts.
Alveolar ducts - lead from the respiratory bronchioles into clusters of alveoli called alveolar sacs.
Alveoli - air sacs of the lungs that bud off like individual grapes of a grape cluster, to increase the surface area for exchange of O2/CO2. If damaged or if they burst/bust open, this results in COPD or emphysema, which can be caused by smoking, asbestos exposure, second-hand smoke exposure, smoke inhalation, long-term mold exposure to a toxic mold, microplastics exposure, and others.
Asthma - a tightening and increase in mucous production of the bronchi
Bronchitis - inflammation of the bronchi
Bronchiolitis - inflammation of the bronchioles
5. LUNGS
Lungs - two lungs are divided into 3 lobes on the right side, and 2 lobes on the left side:
- Superior lobe
- Middle lobe
- Inferior lobe
Apex - rounded superior part of the long
Base - broader inferior part of the lung that rests on the diaphragm
Hilus - area of the lung surrounded by pleura, where the bronchi, lymphatic vessels, and nerves enter or exit the medial side of the lung
Parietal pleura - lines the thoracic cavity wall
Visceral pleura - covers each side of the lung surface
Pleural cavity - space between the two pleural layers that contains pleural fluid
Pleurisy - inflammation of the pleura
Pneumonia - infection of the lungs (bacterial, viral, fungal or parasite)
Pneumothorax - deflation of the lung
Complete Activity 2: Bronchial Tree and Lungs
Complete Reviewing Your Knowledge Questions
Laboratory Exercise: Pulmonary Ventilation, Exercise 25, Pages 299-308, In Conjunction With Carolina Biological Respiratory Dry LabRespiratory System - supplies oxygen needed by body cells and tissues to produce ATP energy for metabolism and removes carbon dioxide produced by metabolic reactions.
Respiration - involves three steps: pulmonary ventilation, external respiration, internal respiration and requires the cardiovascular system to transport oxygen and carbon dioxide throughout the body.
Pulmonary ventilation - breathing; movement of air between the atmosphere and the lungs that occurs when we inhale (inspiration) and exhale (expiration).
A. Pulmonary Ventilation:
Pulmonary ventilation - air moves from an area of higher pressure to an area of lower pressure.
Alveolar pressure - air pressure in the lung.
Lung volume - changes result in changes in alveolar pressure.
1. Changing Thoracic and Lung Volumes:
Diaphragm - dome-shaped muscle that, along with other respiratory muscles, contracts or relaxes, changing the size of the thorax, which, in turn, changes lung volume.
Normal inhalation - caused mainly by contraction of the diaphragm.
Forced inhalation - the contraction of the external intercostals further increases the width of the thoracic cage, raising the ribs, further increasing the lung volume and resulting in a greater volume of inhaled air. This is a deep breath.
Normal exhalation - passive process involving relaxation of the diaphragm and elastic recoil of the chest wall and lungs. The diaphragm relaxes and becomes dome-shaped and decreases the length of the thoracic cavity and thoracic volume, causing air to flow out of the lungs.
Forced exhalation - contraction of the internal intercostals depresses the rib cage. In addition, contraction of the following muscles pushes the diaphragm superiorly, further decreasing thoracic volume and resulting in a greater volume of exhaled air:
Complete Activity 1: Respiratory Muscles and Volume Changes.
Respiration - involves three steps: pulmonary ventilation, external respiration, internal respiration and requires the cardiovascular system to transport oxygen and carbon dioxide throughout the body.
Pulmonary ventilation - breathing; movement of air between the atmosphere and the lungs that occurs when we inhale (inspiration) and exhale (expiration).
A. Pulmonary Ventilation:
Pulmonary ventilation - air moves from an area of higher pressure to an area of lower pressure.
Alveolar pressure - air pressure in the lung.
Lung volume - changes result in changes in alveolar pressure.
- When lung volume increases, the pressure of air inside the lungs decreases and air flows into the lungs.
- When lung volume decreases, the pressure of the air increases and air flows out of the lungs.
1. Changing Thoracic and Lung Volumes:
Diaphragm - dome-shaped muscle that, along with other respiratory muscles, contracts or relaxes, changing the size of the thorax, which, in turn, changes lung volume.
- When relaxed, it is dome-shaped. The diaphragm relaxes and becomes dome-shaped and decreases the length of the thoracic cavity and thoracic volume, causing air to flow out of the lungs.
- When contracted, it flattens, increasing the volume of the thoracic cavity, forcing air into the lungs.
Normal inhalation - caused mainly by contraction of the diaphragm.
Forced inhalation - the contraction of the external intercostals further increases the width of the thoracic cage, raising the ribs, further increasing the lung volume and resulting in a greater volume of inhaled air. This is a deep breath.
Normal exhalation - passive process involving relaxation of the diaphragm and elastic recoil of the chest wall and lungs. The diaphragm relaxes and becomes dome-shaped and decreases the length of the thoracic cavity and thoracic volume, causing air to flow out of the lungs.
Forced exhalation - contraction of the internal intercostals depresses the rib cage. In addition, contraction of the following muscles pushes the diaphragm superiorly, further decreasing thoracic volume and resulting in a greater volume of exhaled air:
- Abdominal muscles:
- External oblique
- Internal oblique
- Transverse abdominis
- Rectus abdominis
Complete Activity 1: Respiratory Muscles and Volume Changes.
2. Pressure Changes During Pulmonary Ventilation:
Thorax - chest cavity
Pleural cavity - increases slightly in volume, causing a decrease in the interapleural pressure, the pressure between the pleural layers.
Intrapleural pressure - the pressure between pleural layers that, when decreased, along with the surface tension of the pleural fluid, causes the visceral pleura and lungs to be pulled outward.
Alveolar pressure - pressure inside the lungs that decreases below atmospheric pressure when lung volume increases, causing air to enter the lungs.
Complete Activity 2: Pressure Changes During Pulmonary Ventilation. Label the model lung bell-jar. Complete table 25.1. Answer the discussion questions regarding the bell jar model lung. Watch the video demonstration below of the model lung demonstration and then complete this activity.
Thorax - chest cavity
- As it expands, the parietal pleura attached to the internal thoracic wall is pulled outward, it increases in size, causing intrapleural pressure and alveolar pressure to decrease, and air enters the lungs.
- As it contracts, it decreases in size, the lungs recoil, causing intrapleural pressure and alveolar pressure to increase, and air leaves the lungs
Pleural cavity - increases slightly in volume, causing a decrease in the interapleural pressure, the pressure between the pleural layers.
Intrapleural pressure - the pressure between pleural layers that, when decreased, along with the surface tension of the pleural fluid, causes the visceral pleura and lungs to be pulled outward.
Alveolar pressure - pressure inside the lungs that decreases below atmospheric pressure when lung volume increases, causing air to enter the lungs.
Complete Activity 2: Pressure Changes During Pulmonary Ventilation. Label the model lung bell-jar. Complete table 25.1. Answer the discussion questions regarding the bell jar model lung. Watch the video demonstration below of the model lung demonstration and then complete this activity.
In the bell-jar model lung, the glass or plastic covering (external surface) represents the parietal pleura and the thoracic wall. The middle tube represents the trachea with the two bronchi (bronchus) branching off of it. The balloons represent the 2 lungs covered with visceral pleura. The inner surface of the jar represents the pleural cavity. The rubber at the bottom of the jar represents the diaphragm muscle.
B. Measuring Lung Volumes With Spirometry:
Lung volumes and capacities - view Table 25.2 to see the definitions of these.
Capacities - combinations of different lung volumes.
NOTE: Volume measurements vary according to:
- Gender
- Age
- Height
- Physical condition
1. Measuring Tidal Volume, Expiratory Reserve Volume, Vital Capacity:
Spirometer - an instrument used to measure lung volumes and capacities. There are many different types that vary on how they measure air volumes and capacities. We typically use a dry, handheld spirometer in A&P.
- Exhale only into this type of spirometer. It does not measure inspiratory air volumes.
Use the videos below of the demonstrations to aid in answering the questions. Base the measured lung volumes and capacities off of the individual in the video and his results. These videos show what a spirometer is and its purpose, then show a demonstration of how to use it. Complete Activity 3: Measuring Lung Volumes and Capacities in your lab manual.
2. Calcuating Inspiratory Reserve Capacity, Inspiratory Capacity, Functional Residual Capacity, and Total Lung Capacity:
Spirometry - the dry handheld spirometer cannot be used to measure inspiratory volumes and capacities, however, IRV, IC, FRC, and TLC can be calculated using measured values for TV, ERV, and VC using 1,200 mL for residual volume (RV). As indicated in Table 25.2, 1,200 mL is average for healthy adults.
Complete Activity 4: Calculating Lung Volumes and Capacities
Spirometry - the dry handheld spirometer cannot be used to measure inspiratory volumes and capacities, however, IRV, IC, FRC, and TLC can be calculated using measured values for TV, ERV, and VC using 1,200 mL for residual volume (RV). As indicated in Table 25.2, 1,200 mL is average for healthy adults.
Complete Activity 4: Calculating Lung Volumes and Capacities