The Urinary System and the Urinalysis:
Lecture Objectives, Chapter 18: Urinary SystemUpon completion of this chapter, you should be able to:
Lab Objectives, Exercise 28: Structure of the Urinary System and Urinalysis and Sheep Kidney DissectionUpon completing these exercises, you should be able to:
- Identify the major organs of the urinary system and give the generalized function of each.
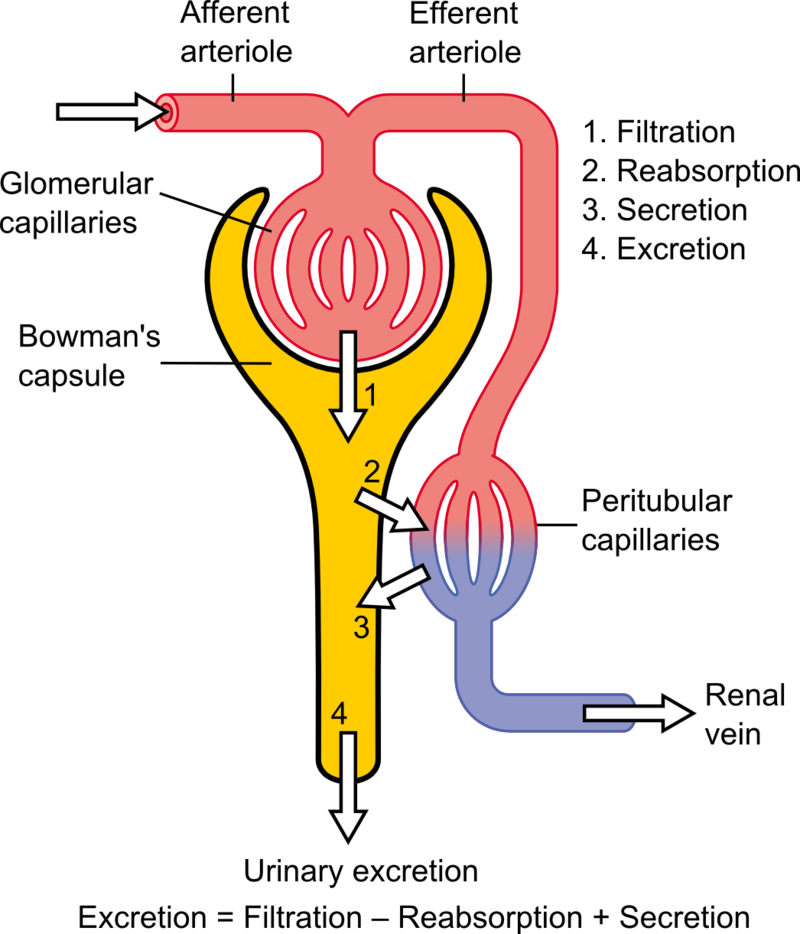
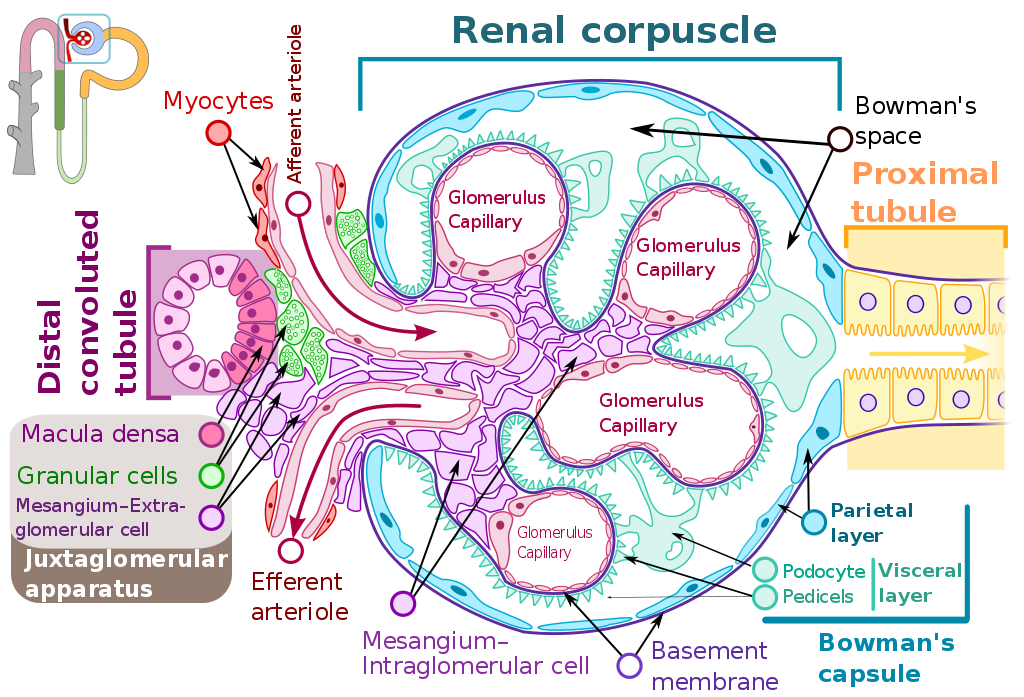
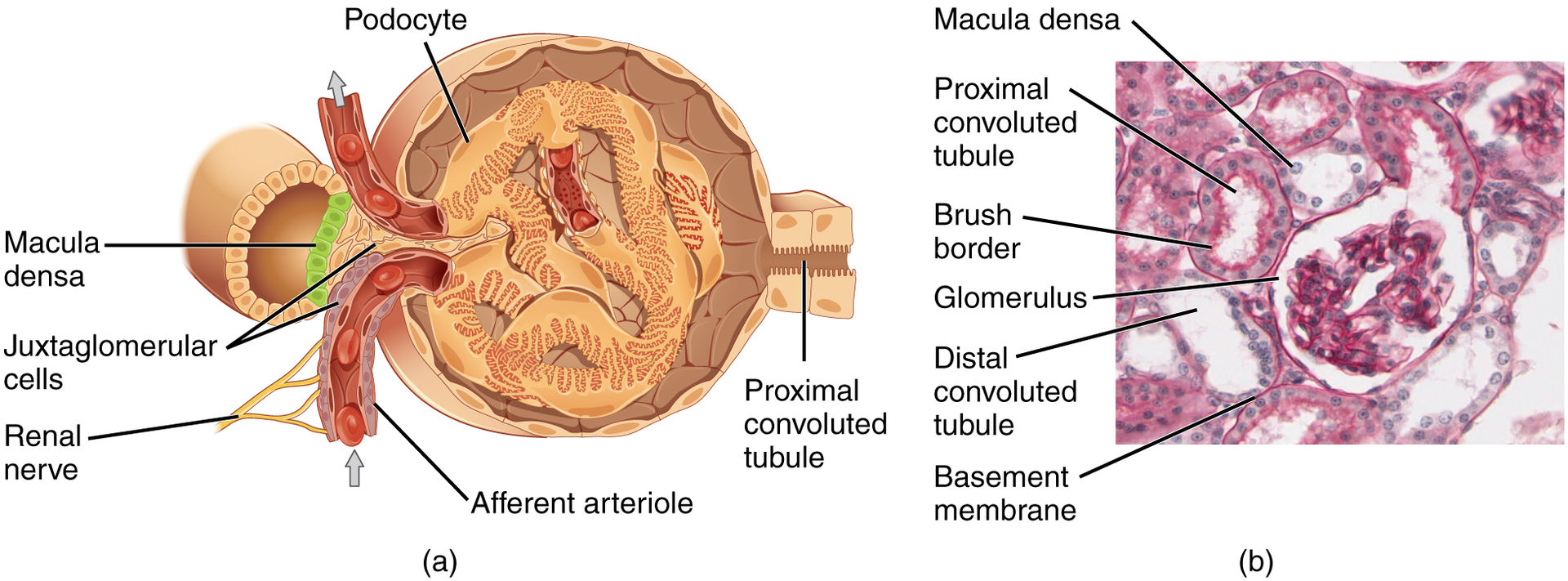
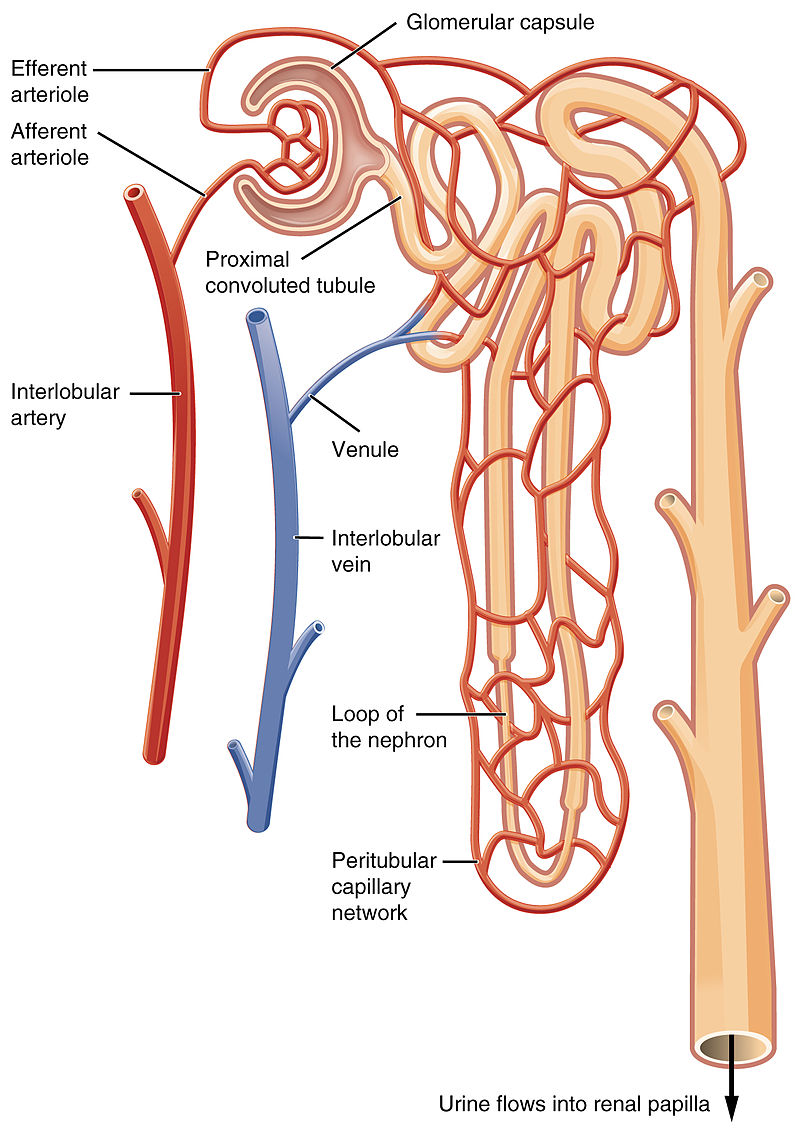
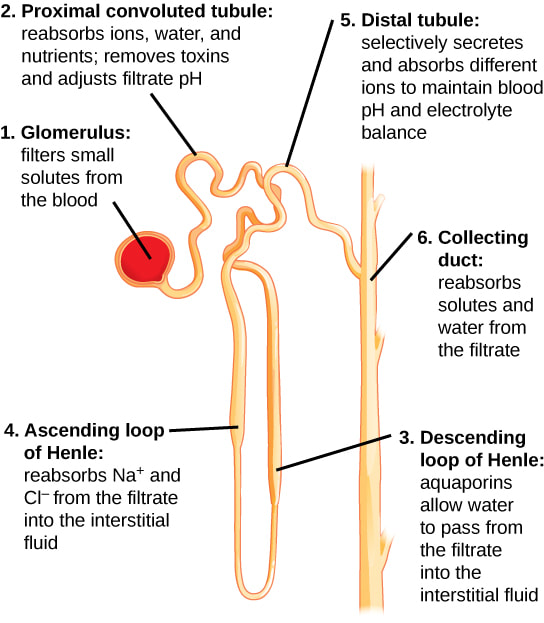
- Name the parts of a nephron and describe the role each component plays in the formation of urine.
- Explain how the kidneys act as vital organs in maintaining homeostasis.
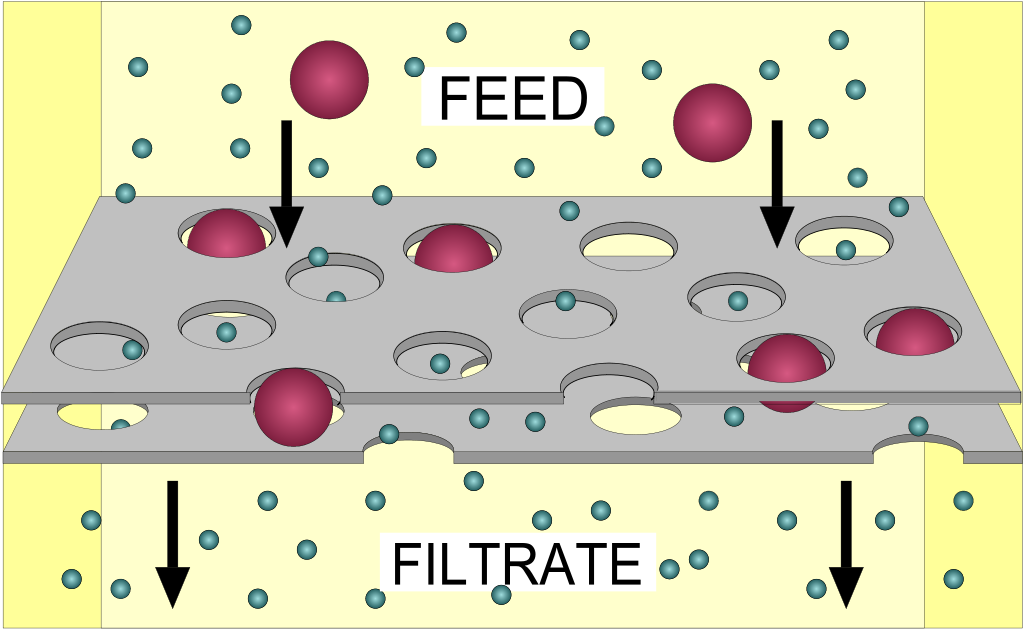
- Explain the importance of filtration, reabsorption, and secretion in urine formation.
- Discuss the mechanisms that control urine volume, including the normal amount and composition of urine.
- Explain the process of urine elimination.
Lab Objectives, Exercise 28: Structure of the Urinary System and Urinalysis and Sheep Kidney DissectionUpon completing these exercises, you should be able to:
- Locate and identify the organs of the urinary system on models or charts.
- Describe how urine is formed.
- Trace the path of urine from formation through the path it takes to the exterior of the body.
- Describe the major features of a urinalysis and its purpose and components.
- Dissect a sheep kidney, identifying the major features of the kidney.
Urinary System:
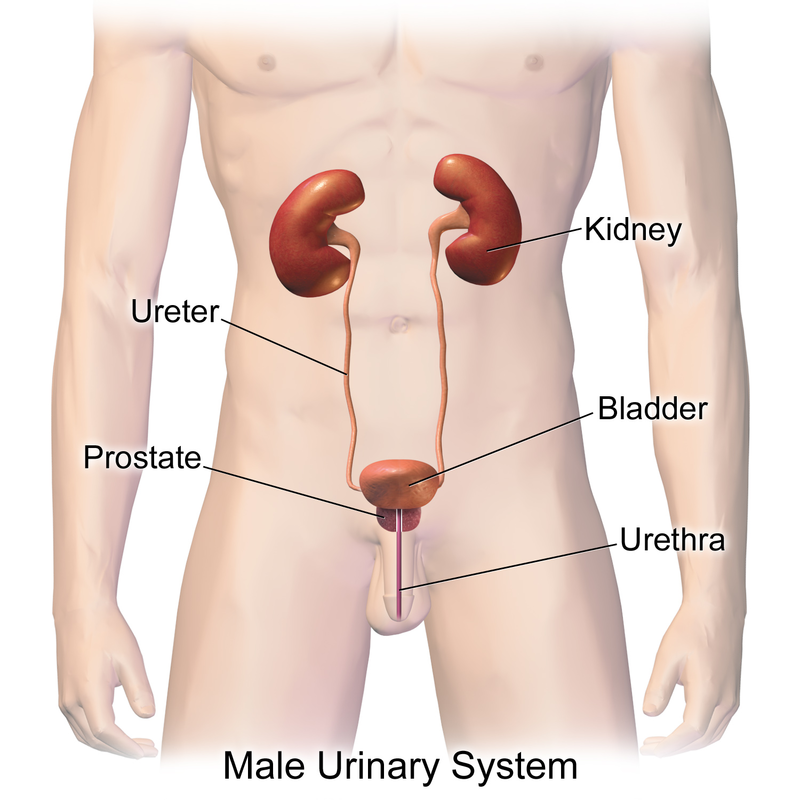
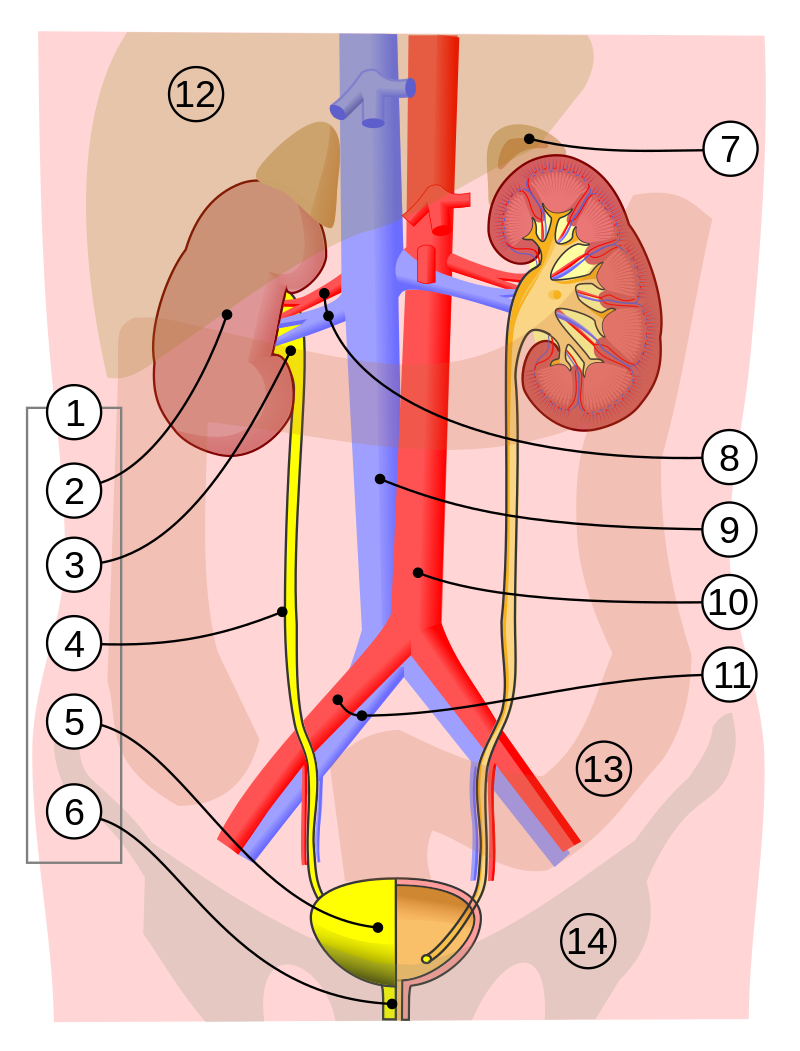
Urinary System Organs: include the kidneys, ureters, urinary bladder, and urethra.
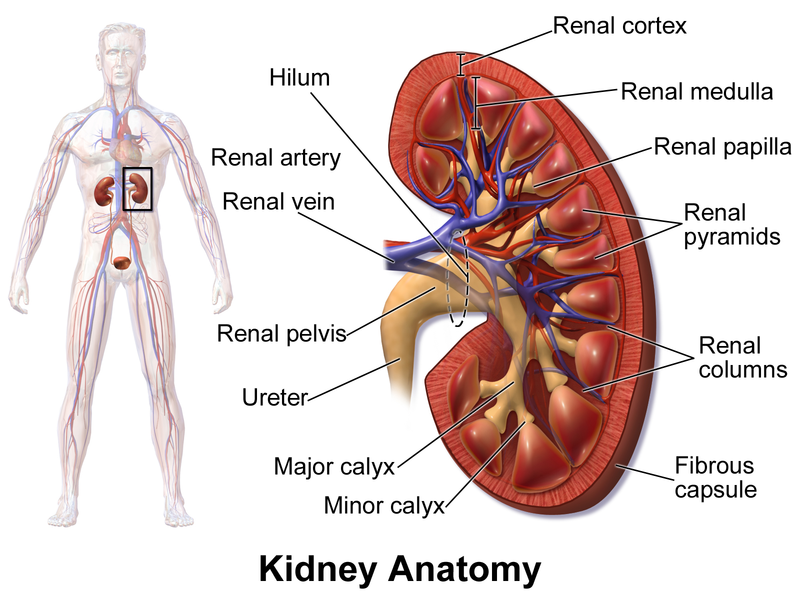
Kidney - regulates water, electrolyte, and pH balance in the body. It removes wastes and nitrogenous substances from blood and excretes them in the urine. They are bean-shaped structures that sit retroperitoneal between the abdominal wall and the peritoneum, are found at the waste level between the 12th thoracic vertebra and the 3rd lumbar vertebra.
Urine - formed in the nephrons of the kidneys and flows through the ureters to the urinary bladder that stores urine until it is eliminated from the body through the urethra.
Retroperitoneal - sitting behind
Renal - pertaining to the kidneys
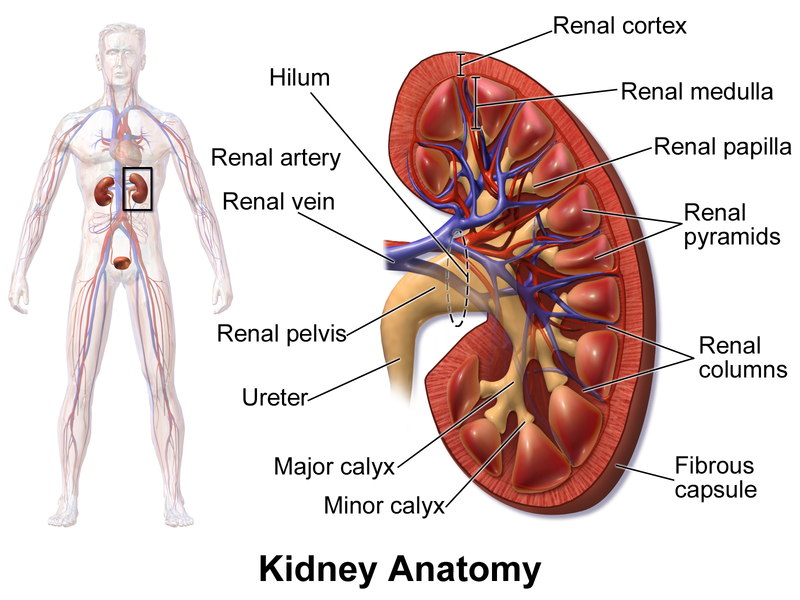
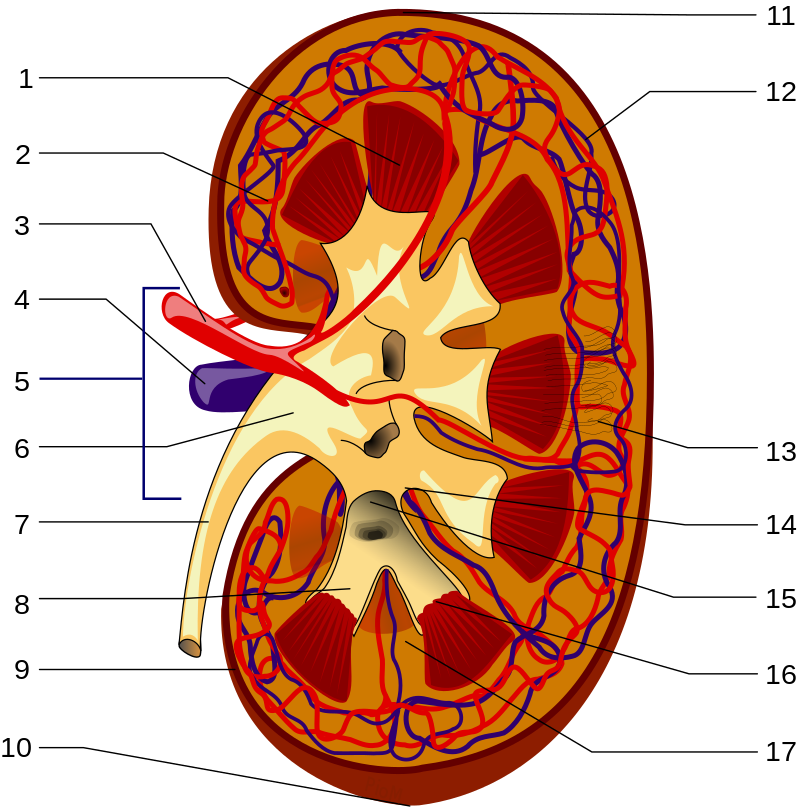
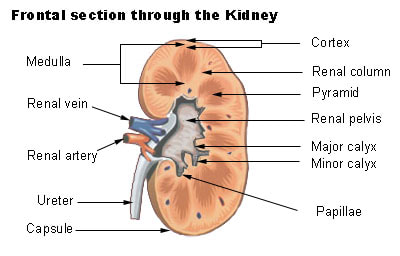
Renal capsule - thin, fibrous membrane that covers the outer surface of the kidney
Renal cortex - the most superficial region of the kidney
Renal medulla - deep to the cortex
Renal pyramids - cone-shaped structures found in the medulla
Renal columns - extensions of the cortex found between the renal pyramids
Base - bottom of each pyramid that faces the cortex
Renal papilla - the apex that is pointed toward the center of the kidney
Nephrons - found in the medulla and cortex, and are the structural and functional units of the kidneys that form urine
Calyces (calyx, singular) - major and minor ducts that exit through openings of the renal papilla and are cup-shaped and carry urine to the renal pelvis
Renal pelvis - urine drains here from the calyces, and it connects to the ureter
Ureters - tubes that drain urine from the renal pelvis to the urinary bladder
Complete Activity 1: Location and Structure of the Kidneys
Urinary System Organs: include the kidneys, ureters, urinary bladder, and urethra.
Kidney - regulates water, electrolyte, and pH balance in the body. It removes wastes and nitrogenous substances from blood and excretes them in the urine. They are bean-shaped structures that sit retroperitoneal between the abdominal wall and the peritoneum, are found at the waste level between the 12th thoracic vertebra and the 3rd lumbar vertebra.
- The right kidney is slightly lower than the left kidney
- The liver forces the right kidney into a lower position
Urine - formed in the nephrons of the kidneys and flows through the ureters to the urinary bladder that stores urine until it is eliminated from the body through the urethra.
Retroperitoneal - sitting behind
Renal - pertaining to the kidneys
Renal capsule - thin, fibrous membrane that covers the outer surface of the kidney
Renal cortex - the most superficial region of the kidney
Renal medulla - deep to the cortex
Renal pyramids - cone-shaped structures found in the medulla
Renal columns - extensions of the cortex found between the renal pyramids
Base - bottom of each pyramid that faces the cortex
Renal papilla - the apex that is pointed toward the center of the kidney
Nephrons - found in the medulla and cortex, and are the structural and functional units of the kidneys that form urine
Calyces (calyx, singular) - major and minor ducts that exit through openings of the renal papilla and are cup-shaped and carry urine to the renal pelvis
Renal pelvis - urine drains here from the calyces, and it connects to the ureter
Ureters - tubes that drain urine from the renal pelvis to the urinary bladder
Complete Activity 1: Location and Structure of the Kidneys
The Ureters, Urinary Bladder and Urethra:
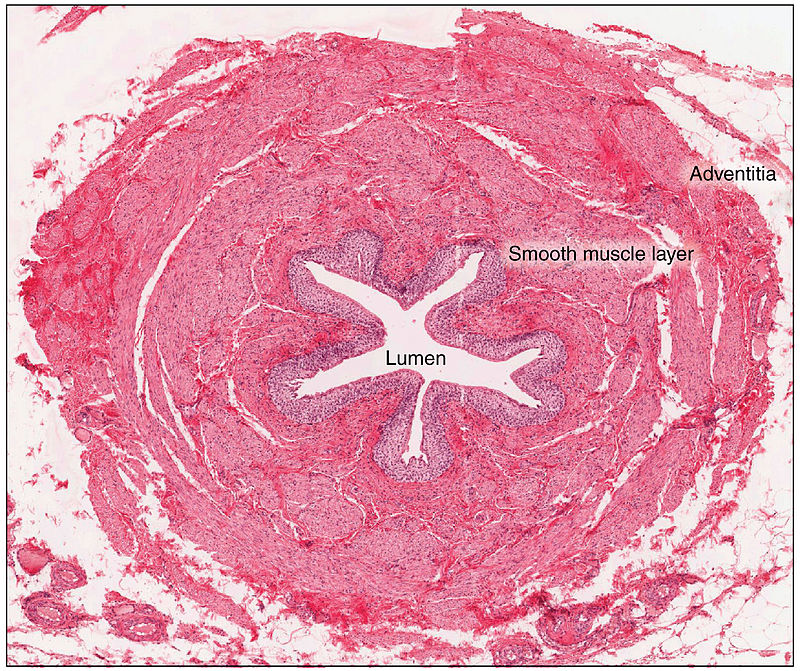
Ureters - narrow, long muscular tubes also located in a retroperitoneal position, descending toward the urinary bladder, curving medially, as they approach the inferior portion of the bladder, and enter the posterior wall of the bladder at an oblique angle.
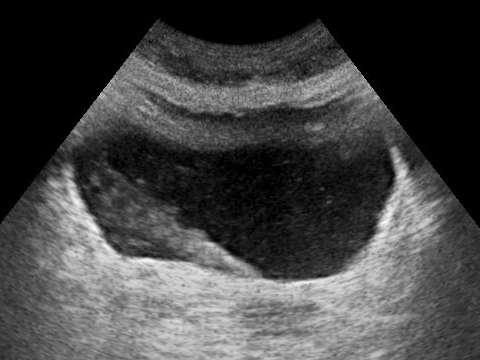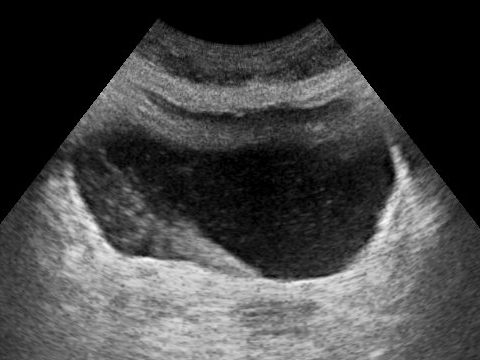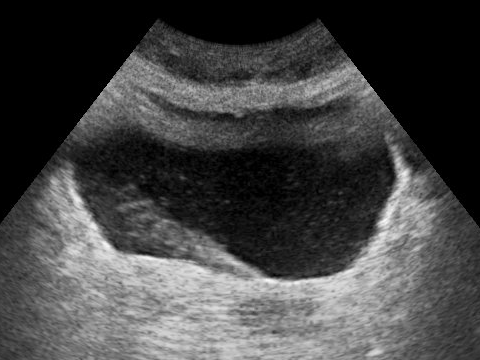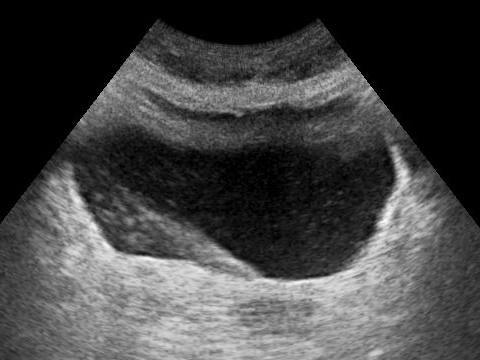
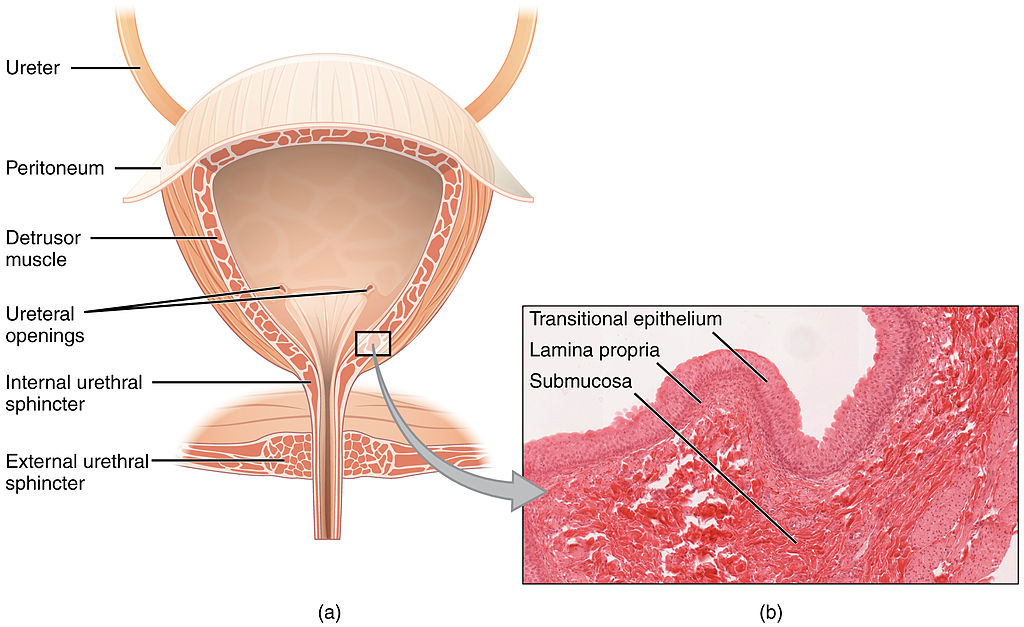
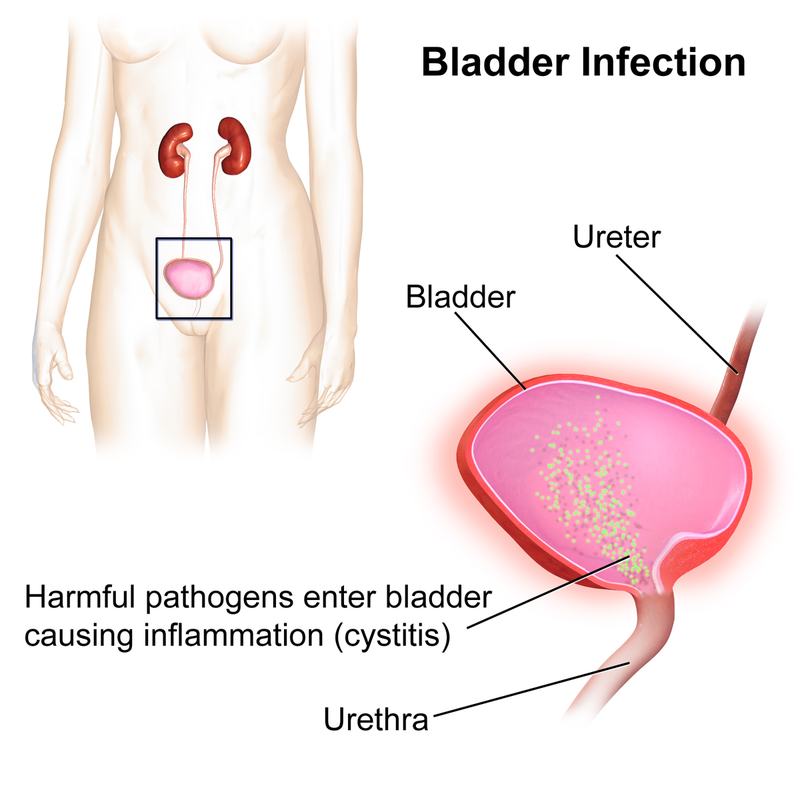
Urinary bladder - a hollow, muscular organ that distends to store urine and has three internal openings that form a triangle called the trigone.
Micturition - urination or voiding.
Internal urethral sphincter - a layer of circular, involuntary smooth muscle that controls passage of urine into the urethra from the urinary bladder.
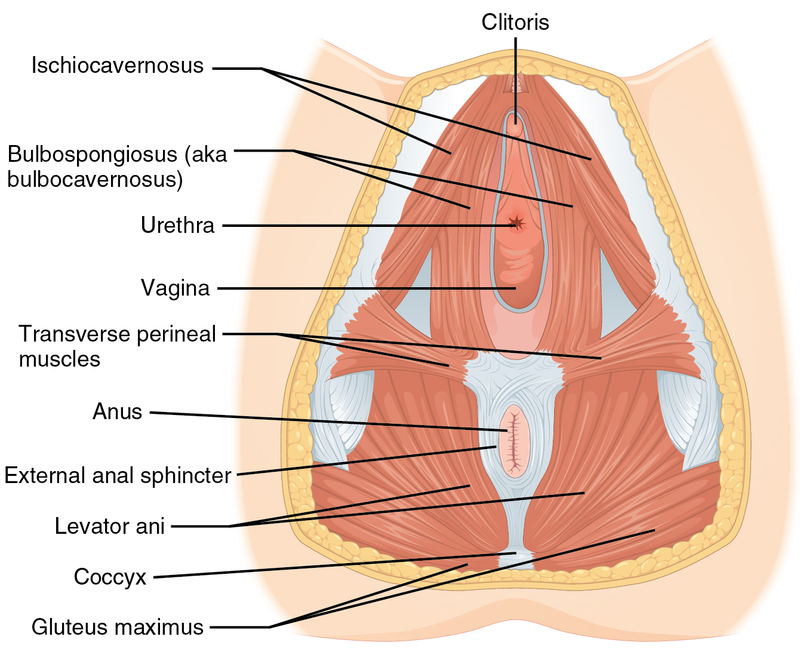
External urethral sphincter - voluntary skeletal muscle within the urogenital diaphragm (deep muscles of the perineum) that permit the passage of urine to the external urethral orifice.
Benign prostatic hypertrophy - a noncancerous enlargement of the prostate gland that restricts the urethra and inhibits urine flow, causing urinary retention.
Ureters - narrow, long muscular tubes also located in a retroperitoneal position, descending toward the urinary bladder, curving medially, as they approach the inferior portion of the bladder, and enter the posterior wall of the bladder at an oblique angle.
Urinary bladder - a hollow, muscular organ that distends to store urine and has three internal openings that form a triangle called the trigone.
- The 2 posterior openings are the ureters.
- The anterior opening is the internal urethral orifice into the urethra.
Micturition - urination or voiding.
Internal urethral sphincter - a layer of circular, involuntary smooth muscle that controls passage of urine into the urethra from the urinary bladder.
External urethral sphincter - voluntary skeletal muscle within the urogenital diaphragm (deep muscles of the perineum) that permit the passage of urine to the external urethral orifice.
Benign prostatic hypertrophy - a noncancerous enlargement of the prostate gland that restricts the urethra and inhibits urine flow, causing urinary retention.
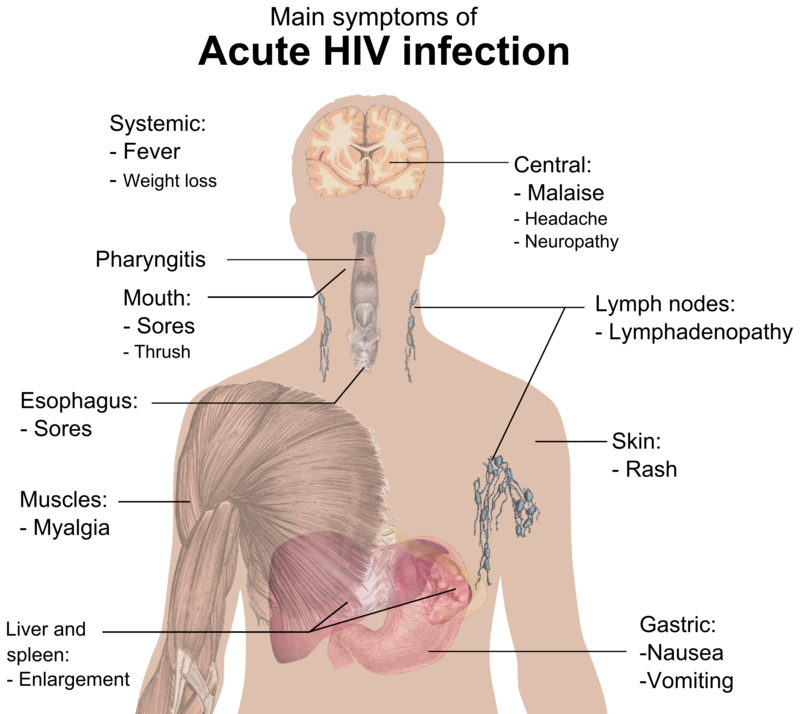
A urinalysis is a group of tests performed to see whether or not the urine is normal or abnormal. Urine can tell a lot about someone's health and underlying conditions, from dehydration, to inability to concentrate the urine, to diabetes, to ketoacidosis, to various types of infections, and much more. A urinalysis panel of tests includes:
- Collection of urine following special protocol, making sure it is properly collected and labeled, making sure it is sealed properly, and sending it to the lab within 2 hours of collection
- Properly preserving the urine until it can be examined
- Macroscopic analysis: color, odor, turbidity, amount/volume, any blood present, dye present, lipids floating, or even kidney stones
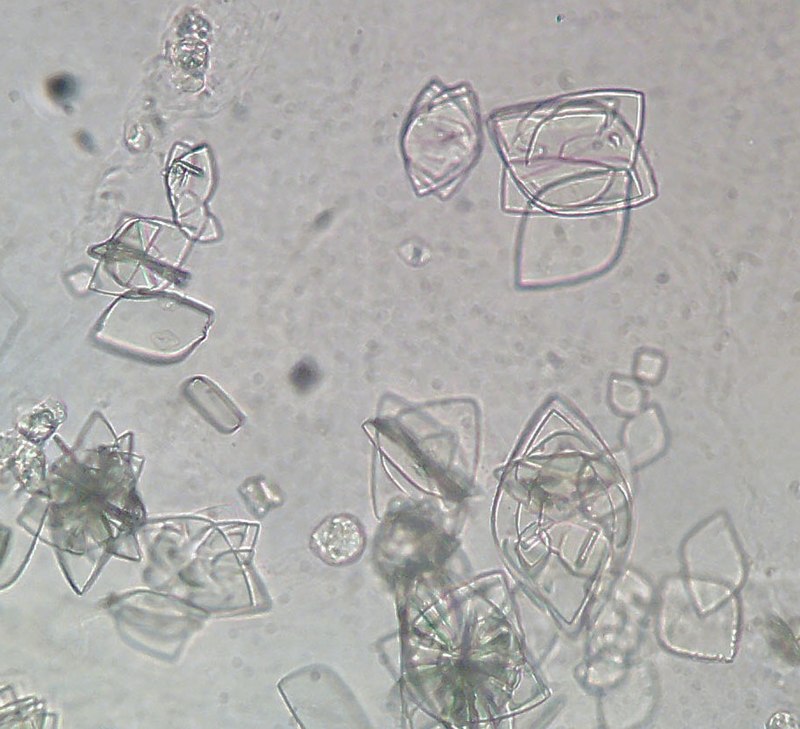
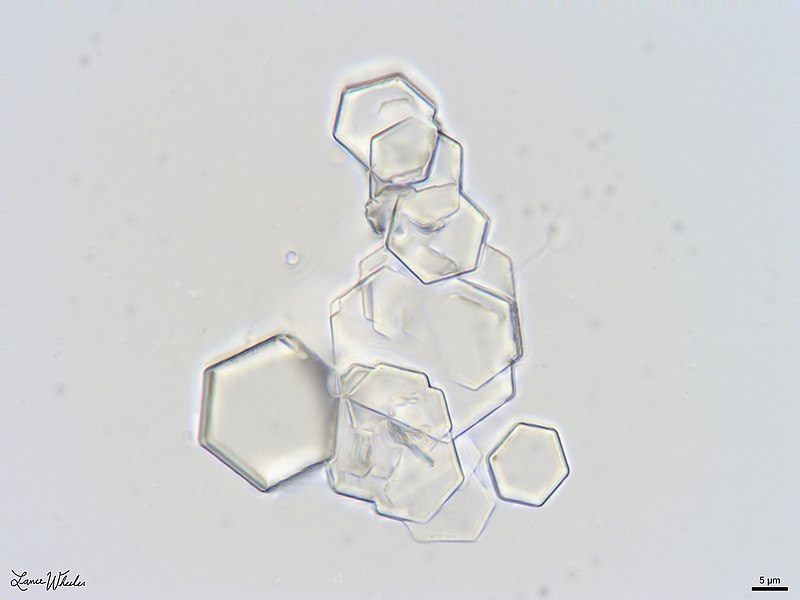
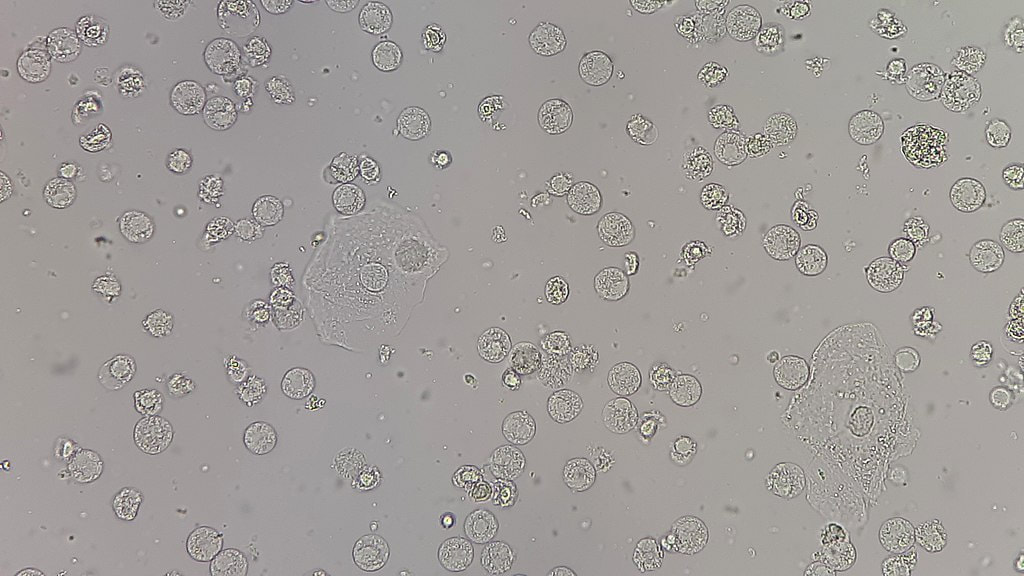
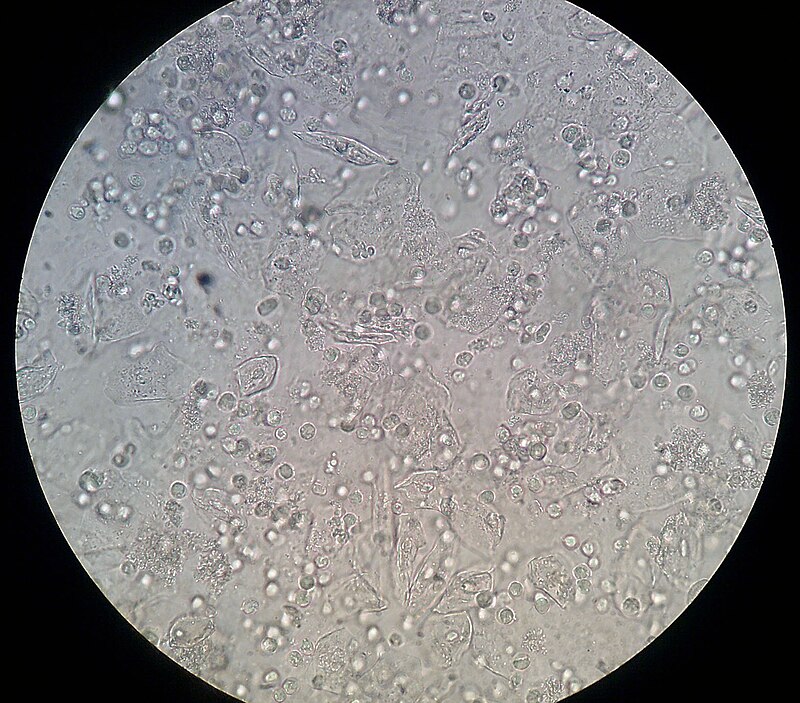
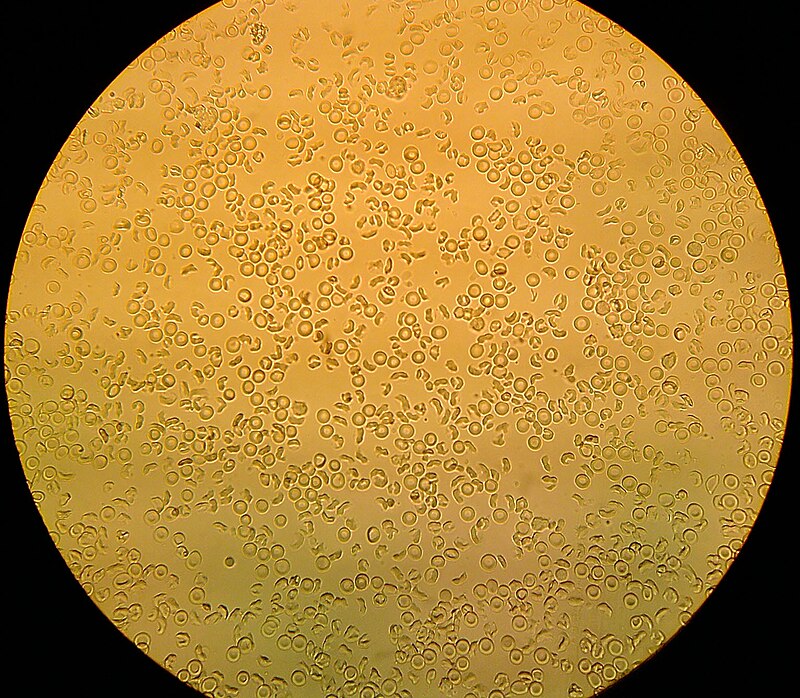
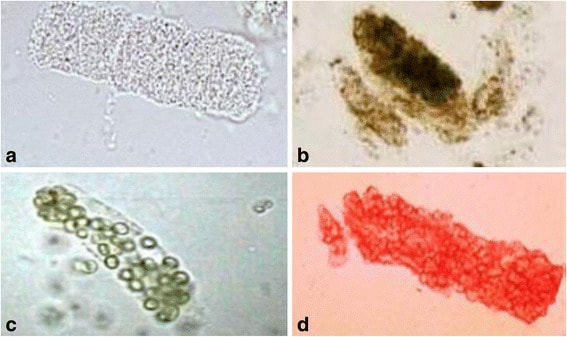
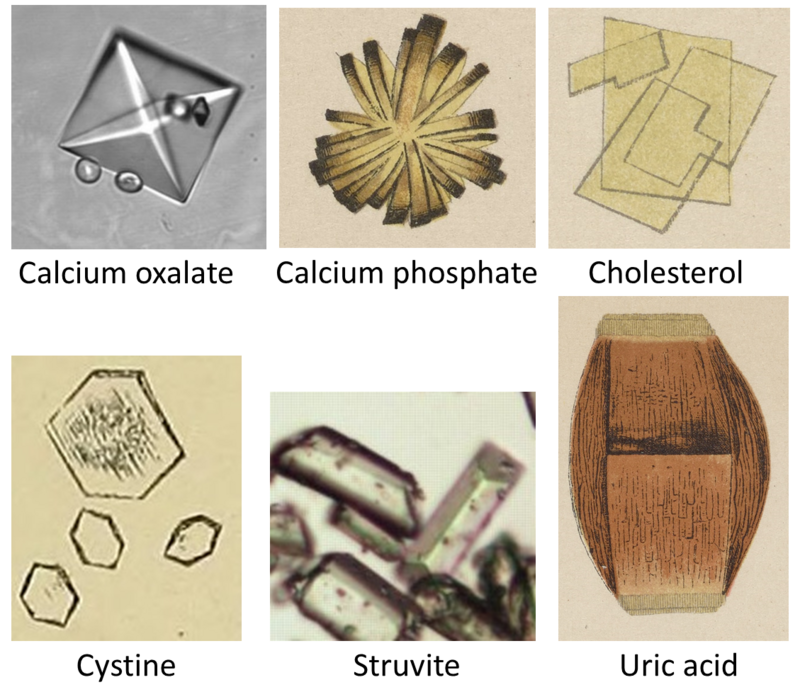
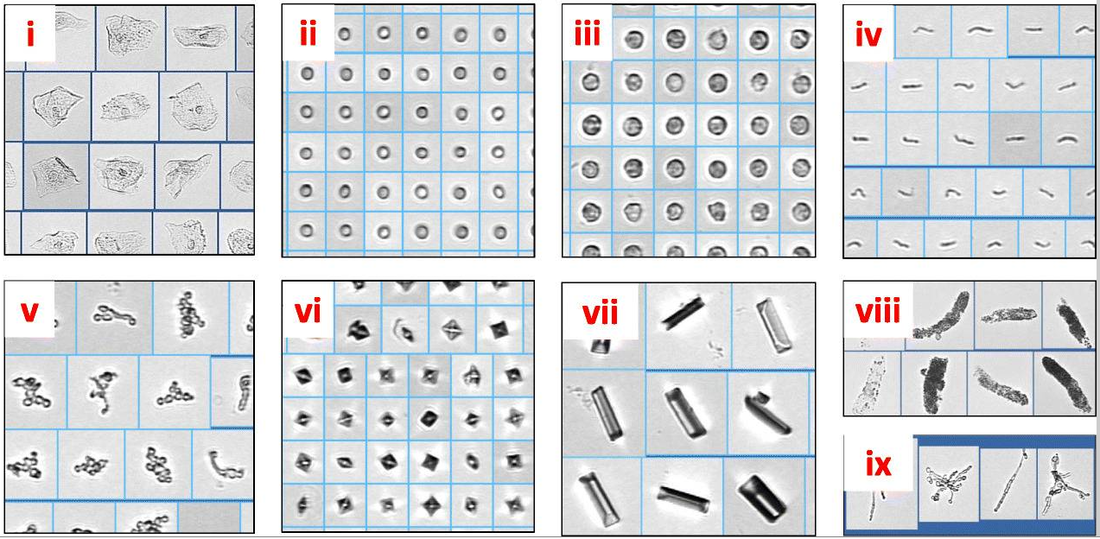
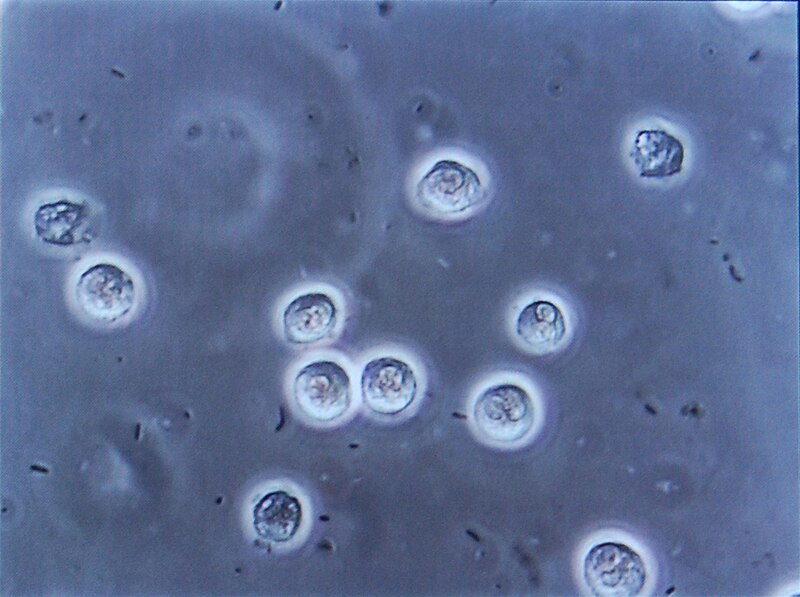
- Microscopic analysis: looking at the urine (following concentration of urine) sediment for the presence of any cells (epithelial, red blood cells, white blood cells/leukocytes), bacteria, yeasts, protists, casts, or crystals
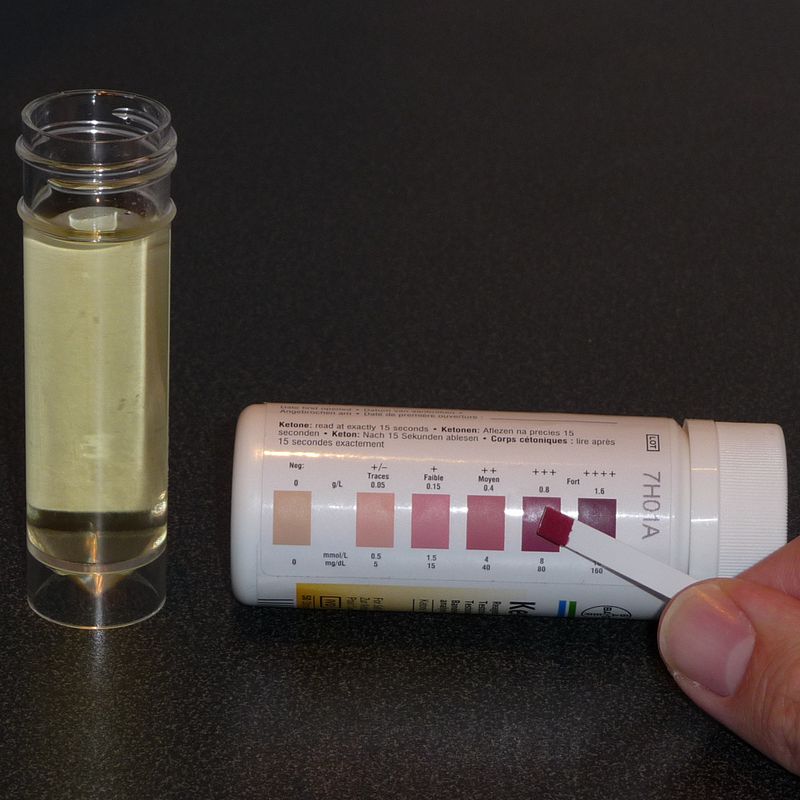
- Multistix dipstix, which test for the presence of glucose, protein, lipids, ketones, bilirubin, urobilinogen, blood, leukocytes, nitrites, and specific gravity
- Specific gravity (can be determined by a urine hydrometer or a test strip or the IRIS automated analyzer)
Urinary System:
Urinalysis:
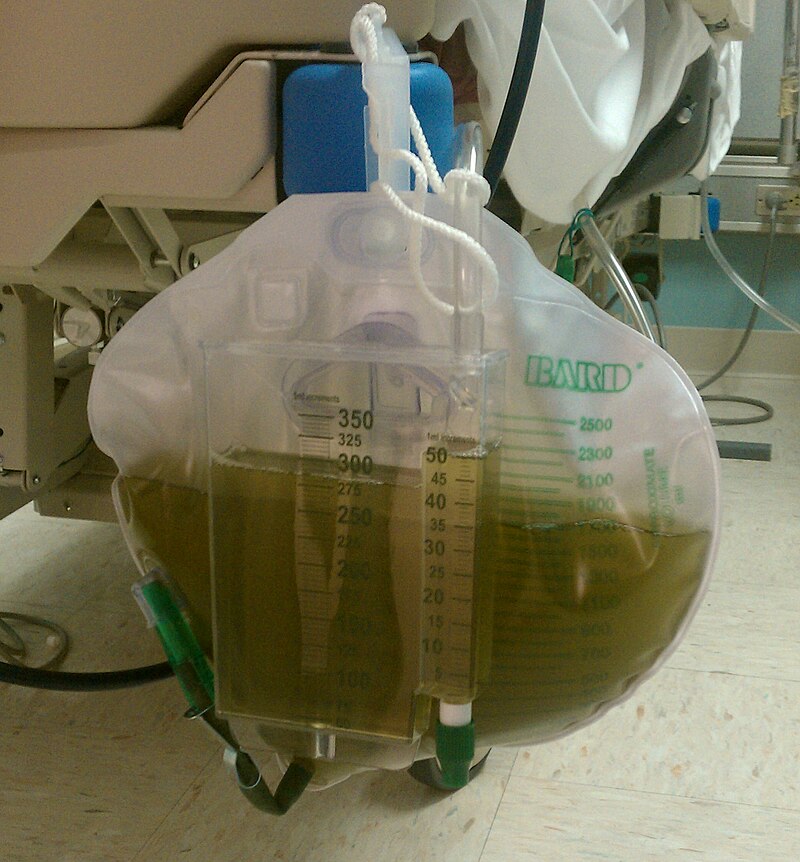
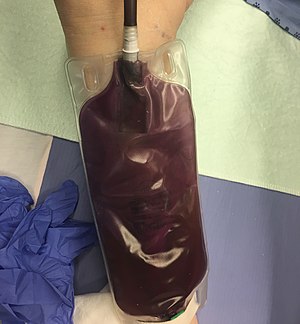
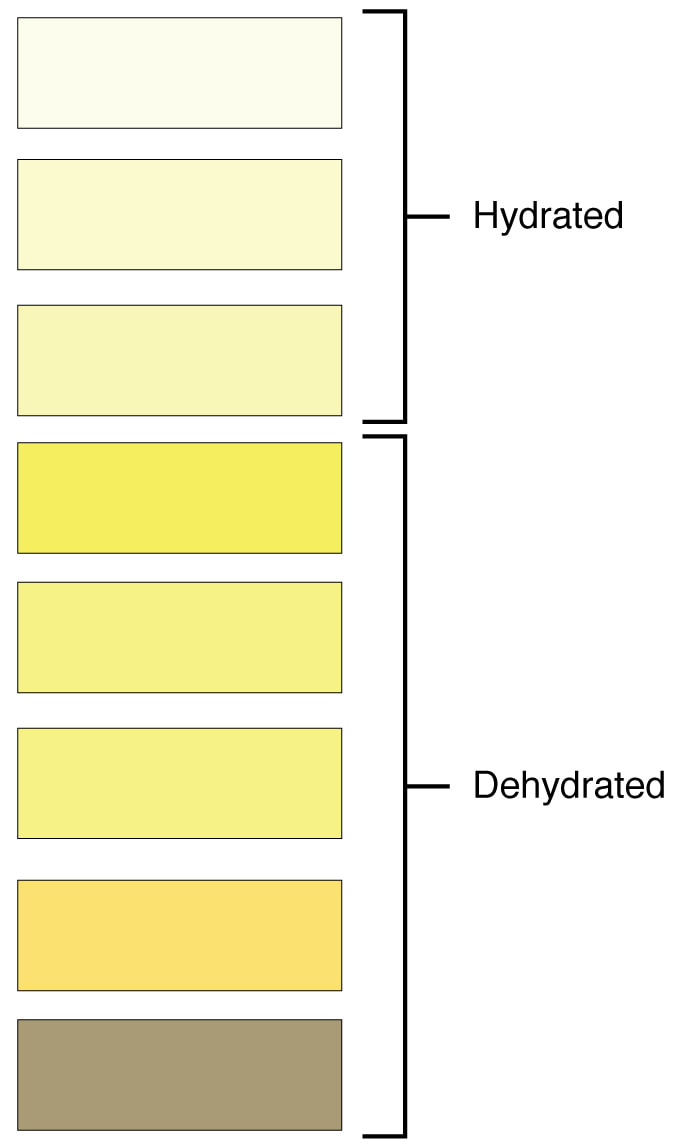
The normal color of urine is a pale straw color, which is a pale yellow, and normal turbidity should be clear. Urine that is darker yellow may signify dehydration, or the need to drink more water. If it is bright neon yellow, this signifies that the individual has taken a vitamin B supplement. If it is too pale, the individual is not concentrating the urine enough. This may or may not be significant. If it is a pattern, it can be significant. Urine that is orange contains bilirubin and sometimes urobilinogen. This could possibly signify liver issues, such as cirrhosis, hepatitis, toxicity, and/or jaundice. If it is cloudy, or turbid, something is in the urine that should not be there. If it is red, it may or may not signify an infection or presence of a kidney stone. If a female is menstruating, it can contaminate the urine with blood. Urine with pus is called pyuria, which is a combination of bacteria, cell debris, and white blood cells. This type of urinary tract infection typically smells very strong, often of ammonia. If the urine is blue, the person likely just had a scan or pyelogram where their veins were injected with blue dye. If the urine is green, they likely have a urinary tract infection with the organism Pseudomonas aeruginosa, a bacterium that produces the green pigment making the urine green. Sometimes consuming a large amount of asparagus can turn the urine green, and consuming a large amount of beets can make it appear red/pink or purple/red.

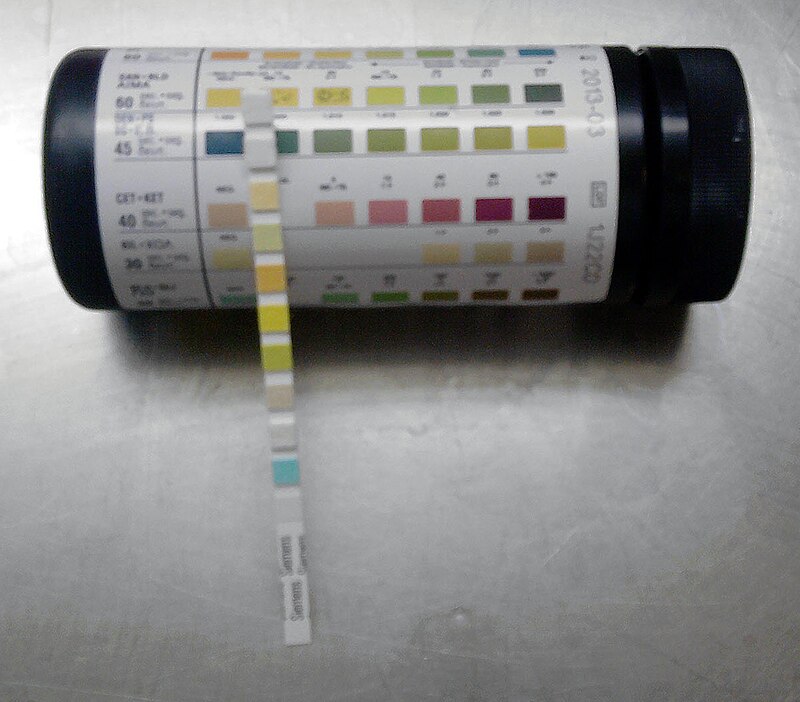
This guide shows the color-coded values to look for when interpreting the multistix urinalysis dip stix. It should be read from the bottom-up, starting with glucose and moving up, reading leukocytes last. The longer part with no pads is designed to serve as a handle to hold the strip. The canister contains this exact color chart for interpretation.
Fluid and Electrolyte Balance:
Lecture Objectives, Chapter 19: Fluid and Electrolyte Balance
Upon completion of this chapter, you should be able to:
Upon completion of this chapter, you should be able to:
- List, describe and compare and contrast the body fluid compartments and their subdivisions.
- Discuss avenues by which water enters and leaves the body and the forces that move fluids into and out of the blood.
- Explain the mechanisms used by the body to maintain fluid balance.
- Discuss the nature and importance of electrolytes in body fluids.
- Describe examples of common fluid and electrolyte imbalances.
- Define the terms fluid balance, electrolytes, ions, electrolyte balance, hypernatremia, hyponatremia, edema, hyperkalemia, hypokalemia, hypercalcemia, hypocalcemia, diuretic, dehydration, overhydration, water intoxication, cations, anions, intracellular fluid, interstitial fluid, extracellular fluid.
Urinalysis:
Urinalysis - an analysis of the physical, chemical, and microscopic characteristics of urine and a measure of urine volume. See Table 28.1 for normal characteristics of urine.
Urine Volume - varies depending on the water content of the body, and decreases when body fluid volume is low.
Specific Gravity of Urine - the weight of a volume of urine divided by the weight of the same volume of distilled water.
Urinalysis - an analysis of the physical, chemical, and microscopic characteristics of urine and a measure of urine volume. See Table 28.1 for normal characteristics of urine.
Urine Volume - varies depending on the water content of the body, and decreases when body fluid volume is low.
Specific Gravity of Urine - the weight of a volume of urine divided by the weight of the same volume of distilled water.
- Urine weight per volume is higher than distilled water because of the presence of solutes in urine.
- The more solutes present in urine (protein, sugar, etc...), the higher the specific gravity.
- Normal urine: 95% water and 5% solutes, including electrolytes, urea, creatinine, uric acid, and metabolic end products of hormones and other substances.
- Electrolytes: sodium, potassium chloride, magnesium, and other ions
- Urea: formed from breakdown of amino acids from proteins
- Creatinine: formed from breakdown of creatine phosphate in muscle tissue
- Uric acid: formed from breakdown of nucleic acids
- Electrolytes: sodium, potassium chloride, magnesium, and other ions
Acid-Base Balance:
Lecture Objectives, Chapter 20, Acid-Base Balance:
- Define the term "acid-base balance" and discuss the concept of pH.
- Define the terms acid, base, buffer, buffer pair, pH, acidosis, alkalosis.
- Compare and contrast strong and weak acids and bases.
- Describe the role of a buffer.
- Contrast the respiratory and urinary mechanisms of pH control.
- Compare and contrast metabolic and respiratory types of alkalosis and acidosis and pH imbalances.
- Discuss compensatory mechanisms that may help return blood pH to near-normal values in cases of pH imbalances.
Lab Objectives, Acidosis and Alkalosis:
Upon completion of this exercise, you should be able to:
Alkalosis and Acidosis Research Lab:Conditions:
Respiratory Acidosis
Respiratory Alkalosis:
Metabolic Acidosis and Diabetic Ketoacidosis:
Metabolic Alkalosis:
Causes:
Signs and Symptoms:
Prevention and Treatment:
pH:
Upon completion of this exercise, you should be able to:
- Differentiate between respiratory alkalosis and acidosis, their causes, and signs and symptoms.
- Differentiate between metabolic alkalosis, metabolic acidosis, and diabetic ketoacidosis, recognize the signs and symptoms, and identify the causes.
- Understand the role of pH, acids, bases, and buffers in the human body.
Alkalosis and Acidosis Research Lab:Conditions:
Respiratory Acidosis
Respiratory Alkalosis:
Metabolic Acidosis and Diabetic Ketoacidosis:
Metabolic Alkalosis:
Causes:
Signs and Symptoms:
Prevention and Treatment:
pH: